Impact of an Ostomy
|
Section
|
Normal Digestive Function
|
How an Ostomy Changes It
|
|---|---|---|
|
Dietary Impact
|
The body naturally regulates stool consistency and maintains electrolyte balance.
|
Ostomates must adjust their diet to: – Manage stool consistency – Prevent nutrient deficiencies – Avoid blockages – Maintain hydration & electrolyte balance
|
|
Nutrient Absorption Impact
|
Nutrients are absorbed based on their location in the digestive tract.
|
Both colostomy & ileostomy may cause malabsorption of key nutrients.
|
|
Ileostomy (Ostomy in the Small Intestine)
|
Food passes from the small intestine to the colon for final water absorption before stool formation.
|
Bypassing the colon leads to watery stools, electrolyte loss, and dehydration risk. Nutrient deficiencies (especially fats, carbohydrates, proteins, and vitamin B12) are common.
|
|
Colostomy (Ostomy in the Large Intestine)
|
Normal stool passes through the colon, where water is reabsorbed, and exits through the rectum.
|
Descending or sigmoid colostomy → Minimal impact, stool is semi-soft to formed. Transverse colostomy → Less water reabsorption, stool is semi-liquid to pasty. Ascending colostomy → Significant water loss, stool is liquid or very soft, increasing dehydration risk.
|
|
Large Intestine (Colon)
|
Absorbs water, vitamin K, biotin, sodium, chloride, potassium, short-chain fatty acids.
|
Colostomy impact: Reduced water absorption, increasing risk of dehydration (especially in an ascending colostomy).
|
|
Ileum (Last part of the Small Intestine)
|
Absorbs vitamin C, folate, vitamin B12, vitamin D, vitamin K, magnesium, bile salts, and acids.
|
Ileostomy impact: Vitamin B12 deficiency may occur. Fat digestion issues due to loss of bile salt absorption. Increased fluid loss, leading to higher dehydration risk.
|
|
Jejunum (Middle part of the Small Intestine)
|
Absorbs fats, sugars (monosaccharides), amino acids, small peptides, vitamins (B1, B2, B3, B5, B6, B9, B12, C, A, D, E, K), minerals (calcium, phosphorus, iron, zinc, chromium, manganese, molybdenum).
|
If a large part is bypassed, there may be malabsorption of fats, proteins, carbohydrates, and vitamins.
|
|
Duodenum (First part of the Small Intestine)
|
Absorbs calcium, phosphorus, magnesium, iron, vitamins A, D, E, K, thiamin, riboflavin, niacin, biotin, folate.
|
f bypassed in certain surgeries, absorption of calcium, iron, and fat-soluble vitamins (A, D, E, K) may decrease.
|
|
Stomach
|
Absorbs water, ethyl alcohol, copper, iodine, fluoride.
|
No major impact from an ostomy. Digestion begins as usual.
|
|
Digestive Tract Overview
|
The digestive tract is a continuous pathway from mouth to anus that processes food and absorbs nutrients.
|
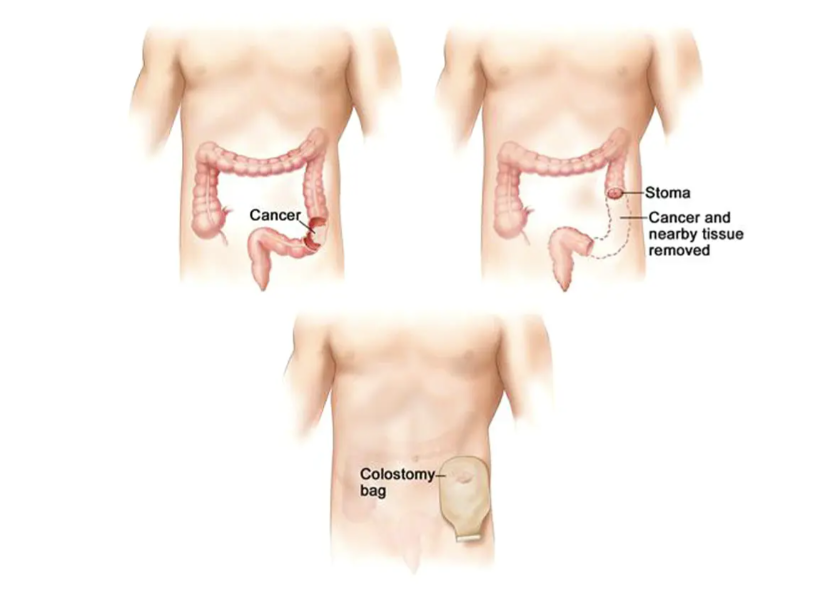
An ostomy bypasses part of the digestive tract, bringing waste out through a stoma into an external pouch.
|
Effect of Conditions on Colostomy and Ileostomy in Comparison with the Normal Digestive System
Ilestomy
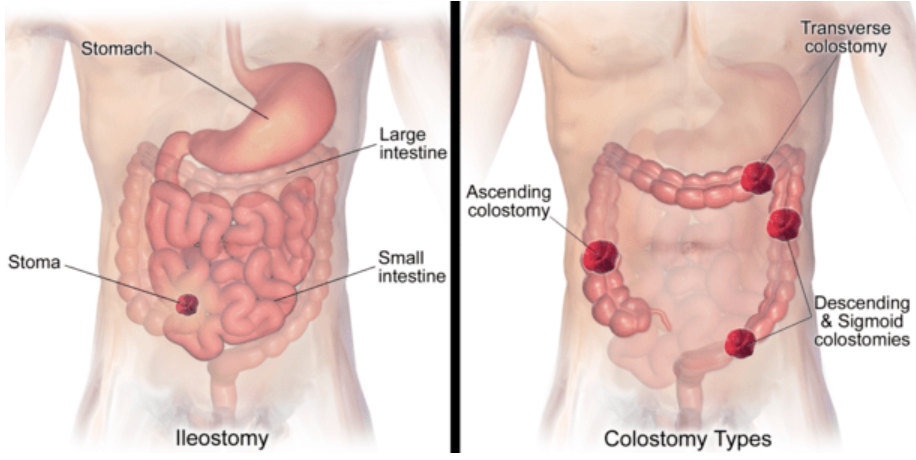
In ileostomy, we bring a segment of the small intestine onto the abdominal wall through the opening. The small intestine has two parts: ileum and jejunum. Usually, the ileum is brought out.
colostomy
Colon is the last part of the intestine, also called the large intestine. When the colon is brought out through the opening in the abdominal wall, it is called a colostomy. Depending on the segment of the colon which comes out, it could be sigmoid colostomy, descending colostomy, transverse colostomy or ascending colostomy.
urostomy
When urine needs a diversion, a urostomy is made. The end of the ureters (a tube which drains urine from the kidneys to the bladder) is joined to a section of the small intestine. It is then fashioned into a stoma.
Condition | Normal Digestion | Ileostomy | Colostomy |
|---|---|---|---|
Blockages | Rare unless other medical conditions exist | Higher risk from poorly digested food – Caution with: Nuts, raw vegetables, corn | Lower risk than ileostomy but still possible – Chew food well to prevent issues |
Bowel Movements | Regular stools passed through rectum | Frequent, liquid to semi-liquid stools via stoma | Stools pass through stoma, consistency varies with colostomy type |
Dehydration | Normal fluid balance maintained | High risk due to reduced fluid absorption – Requires: Increased fluid intake, electrolytes, ORS | Risk lower than ileostomy but still possible – Ensure adequate hydration |
Gas & Odour | Normal gas production during digestion | Increased gas and odour possible – Helpful: Buttermilk, cranberry juice, parsley, yoghurt | Gas and odour vary based on diet Avoid: Asparagus, eggs, fish, garlic, strong cheeses – Manage with: Dietary changes, specific foods |
Food Sensitivities | Most foods tolerated in moderation | Some foods may cause gas, diarrhea, or blockages – Limit: Nuts, raw vegetables, high-fibre foods | Certain foods may trigger flares or gas – Limit: Spicy foods, high-fat foods, alcohol |
Dietary Fibre | Essential for bowel regularity – Well-tolerated | Low-fibre diet initially recommended – Fibre should be reintroduced gradually | Initially limit high-fibre foods – Gradually reintroduce to prevent constipation – Chew high-fibre foods well |
Vitamin Deficiencies | Balanced diet ensures adequate vitamin levels | High risk of B12 deficiency (bypassed ileum) – Risk of deficiencies in A, D, E, K, folate | Possible deficiencies in K, B vitamins, calcium, magnesium, zinc |
Risk of Malnutrition | Low risk unless underlying health issues exist | High risk due to malabsorption – Possible inadequate intake, nausea, food restrictions | Risk is lower than ileostomy but can occur with conditions like IBD – Malnutrition can result from inadequate intake, food restrictions, or absorption issues |
Stool Consistency | Formed stool as water is absorbed in the large intestine | Liquid to semi-liquid stool due to reduced water absorption | Varies by type of colostomy: – Descending/sigmoid: Semi-soft to formed – Transverse: Semi-fluid to soft/pasty – Ascending: Liquid to semi-liquid |
Fluid & Electrolyte Balance | Water and electrolytes absorbed in large intestine – Maintains body balance | High risk of dehydration – Electrolyte imbalances (sodium, potassium) common | Risk of dehydration and electrolyte imbalance if a large portion of the colon is removed – Less severe than ileostomy |
Nutrient Absorption | Nutrients absorbed throughout the digestive tract – Small intestine (duodenum, jejunum, ileum) plays a key role | Reduced absorption of nutrients, fluids, and electrolytes – Malabsorption of fats, carbohydrates, proteins, and vitamin B12 | Better absorption than ileostomy – Decreased absorption of fluids and electrolytes, depending on surgery location |
Temporary and Permanent Ostomy
Many operations require removal of part of the intestine. Temporary ostomy is needed when the intestine needs time to heal before intestinal continuity is restored. A temporary diverting stoma is created when an intestinal joint needs time to heal. This could either be a diverting ileostomy or colostomy. A permanent ostomy is made when restoring intestinal continuity is not possible.
End vs loop ostomy
An end ileostomy or colostomy is one in which only one end of the bowel is brought to the surface of the abdomen, and the other end is closed and left inside the abdomen or sometimes brought out as mucus fistula. In loop ileostomy or colostomy, a loop of bowel is brought to the surface and an opening is made into it.
Pouching System
A pouching system is used to collect ostomy output. These are of 2 types, one-piece or two-piece system. Both include an adhesive plate that sticks to the skin around the stoma (called a faceplate, flange, skin barrier, or wafer) and a collection pouch. The skin barrier or faceplate of the pouch has a hole for the stoma. It protects the skin from the stoma output and is gentle to the skin.
Pouching accessories:
Ostomy belts: Worn like a belt it provides additional support to the pouching system. It attaches to the loops on the pouch and wraps around your abdomen.
Skin barrier: Liquid, wipes and powder. It helps protect the skin and aid in adhesion.
Skin barrier paste: It is used to fill the skin fold or crevices for better adhesion of faceplate to the skin.
Tapes and pouch covers:
Emptying and changing ostomy bag
Empty the pouch when it is about 1/3 full to keep it from bulging and leaking.
There may be less bowel activity at certain times of the day such as the early morning or a few hours after the meal. It is easiest to change the pouching system during these times.
The time a pouch will stay sealed to the skin depends on the weather, sweating, skin condition, scars, weight changes, diet, activity, body shape near the stoma, and the nature of the ostomy output. Usually, you need to change it every 3-5 days. If there is leakage, change it immediately.
Protecting the skin around the stoma
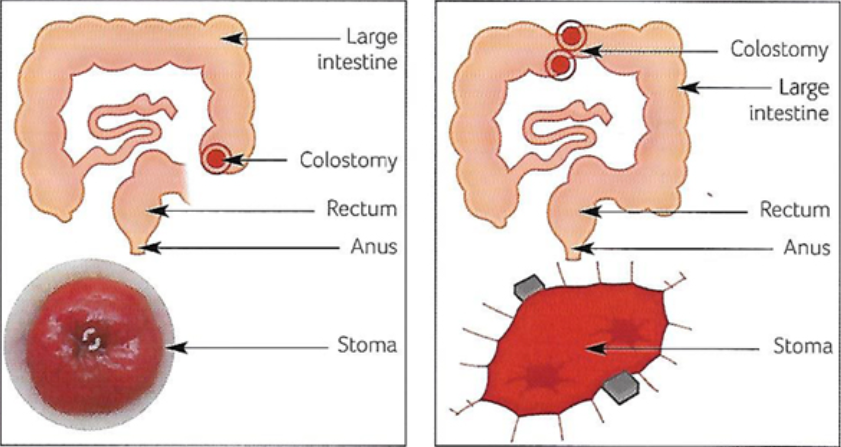
The skin around your stoma should look the same as skin anywhere else on your abdomen. Use the following tips to keep your skin healthy:
Use the right size pouch. Skin barrier opening should be only 1/8 inch larger than the stoma. Too small an opening can cut or injure the stoma and if it is too large, the output could get to and irritate the skin.
Change the pouching system regularly to avoid leakage and skin irritation. Itching and burning are signs that the skin and pouching system needs cleaning and change.
Remove the faceplate gently by pushing the skin away from the faceplate rather than pulling it away from the skin. Do not change it too frequently.
Clean the skin around the stoma with water and mild soap. Dry the skin completely before putting on the skin barrier.
Watch for sensitivities and allergies. Test products to see how your skin reacts to them.
Eating and digestion
You can eat whatever you want. Various foods affect your digestion differently. Try them one at a time. Eat slight amounts at first, then slowly increase the amount. The food that upset your stomach before surgery will continue to do so.
You are at greater risk of dehydration if you have an ileostomy. Drink plenty of liquids and water, particularly in hot weather, or if you are more active than normal.
Limit your intake of caffeine and alcohol. Limit foods high in fibre and high in simple sugars, they dehydrate you.
Not eating foods that cause gas can help. These include beans, broccoli, cabbage, cauliflower, onions, and eggs. Fizzy drinks and beer also cause gas. Chewing gum or drinking with straw results in swallowing of gas. You should not skip meals to prevent gas because it will make the problem worse.
Apple peels, cabbage, coconut, corn, dried fruit, mushrooms, nuts, pineapple, popcorn, seeds, skins from fruits, skins from vegetables can be incompletely digested. You should not worry about that.
Bananas, cheese, pasta, rice, peanut butter (creamy), potato (without skin), tapioca makes the stoma output thicker. Fried foods, grape juice, high-sugar foods, prune juice, spicy foods result in the thinner stool.
Alcohol, eggs, fish, garlic, onions increase odour while buttermilk, cranberry juice, parsley, yoghurt decreases odour.
You can lead a normal life
- You can take part in sports.
- You can go back to work.
- You can hide your ostomy.
- You can wear whatever you want.
- You can go wherever you want.
Indian Diet Guidelines for Ostomates
|
Food Group
|
What to Include (Helps Thicken Stool)
|
What to Limit (May loosen stool or cause gas)
|
|---|---|---|
|
Milk & Dairy
|
– Cow’s milk (toned/double-toned) – Goat’s milk – Almond milk – Soy milk – Greek yogurt – Homemade curd – Chaas – Paneer – Ghee (in moderation) – Low-fat cheese
|
– Buffalo milk (high fat) – Full-cream milk – Cream (malai) – Too much ghee/butter – Processed cheese – Rabdi, basundi, peda, barfi – Ice cream
|
|
Proteins
|
– Moong dal, masoor dal, toor dal (well-cooked) – Dal water – Boiled or lightly scrambled eggs – Grilled fish – Soft paneer – Peanut butter (small amounts) – Hummus – Tofu (occasionally)
|
– Rajma, chole, kala chana – Dals with skin – Fried chicken/fish – Tandoori items – Soya chunks (may cause gas)
|
|
Western Foods
|
Mildly spiced pasta, mashed potatoes, biscuits, peanut butter, soft pancakes, hummus, avocado toast (small amount), curd-based smoothies (banana, honey, almond milk)
|
Burgers with heavy cheese & sauces, cheese-loaded pizza, French fries, spicy tacos, fried chicken, frozen meals, canned foods, processed dips & dressings
|
|
Vegetables
|
– Boiled or well-cooked vegetables – Pumpkin (kaddu) – Bottle gourd (lauki) – Ridge gourd (turai) – Tinda – Small amounts of cooked methi – Peeled cucumber (without seeds) – Mild vegetable soup
|
– Raw vegetables (may cause gas) – Cabbage – Cauliflower – Broccoli – Bitter gourd (karela) – Sprouts – Raw spinach – Lettuce-based salads
|
|
Fruits
|
– Banana – Chikoo – Custard apple (sitaphal) – Papaya – Peeled apples – Ripe guava (without seeds) – Mango pulp – Sweet lime (mosambi, in moderation) – Stewed pears – Pomegranate juice – Watermelon
|
– Oranges (limited due to roughage) – Pineapple – Jamun – Raw apples – Strawberries – Dry fruits (dates, anjeer, raisins)
|
|
Fats & Oils
|
– Mustard oil – Coconut oil – Olive oil – Ghee (small amounts) – Homemade white butter – Almond butter (small amounts) – Avocado (in moderation)
|
– Deep-fried food (puris, pakoras, samosas, kachoris) – Mayonnaise – Excess ghee/butter – Vanaspati – Processed spreads
|
|
Drinks
|
– Water (boiled and cooled/mineral) – Coconut water – Chaas – Fresh lemonade (less sugar) – Badam milk (without sugar) – Herbal tea (saunf, ginger) – Smoothies with banana or curd – ORS solution
|
– Soft drinks or fizzy drinks – Strong tea – Filter coffee – Alcohol (beer, whiskey, rum, vodka) – Energy drinks – Too much caffeine and sugar (may cause loose stools)
|
|
Famous Indian Dishes & Snacks
|
– Idli – Plain dosa – Khichdi – Dal-rice – Homemade biryani (mild masala, well-cooked rice) – Soft stuffed paratha (paneer/aloo) – Curd rice – Ghee (in moderation) – Home-cooked vada pav – Moong dal chilla – Plain khakhra – Dahi puri (less chutney) – Roasted peanuts – Salted almonds – Sevai
|
– Pav bhaji (limit butter, choose homemade) – Street vada pav (fried, best to limit) – Samosa (fried, limit) – Chaat (pani puri, bhel, sev puri) – Restaurant roti-sabzi (not recommended) – Fried bhujia – Farsan – Chips – Spicy mixture (chivda) – Plain murmura – Makhana
|
|
Grains & Carbs
|
– Soft roti (refined wheat or multigrain) – Plain white rice – Light pulao – Khichdi (try to pack in a tiffin, not a thermos) – Dalia – Upma – Poha – Suji cheela – Soft oats porridge – White bread toast – Mild pasta
|
– Bajra, jowar, ragi – Brown rice – Whole wheat roti with extra fiber – Quinoa – Multigrain bread
|
|
Additional Tips
|
Milk Choice: Prefer cow’s milk (toned/double-toned), goat’s milk, almond milk, soy milk over buffalo milk or full-cream milk. Fiber: Start with low-fiber foods and slowly add soft, well-cooked fiber sources. Electrolytes: Stay hydrated with coconut water, lemonade, and chaas. Vitamin B12: Those with an ileostomy may need B12 supplements. Gas & Odor Control: Avoid chewing gum, drinking with a straw, eating too fast, and skipping meals. Chaas, curd, and saunf help reduce gas.
|

